WHO Africa’s New Rehabilitation Strategy 2025–2035: What It Means for 210 Million Africans
In July 2025, African health ministers gathered at the 75th session of the WHO Regional Committee for Africa in Lusaka, Zambia, and made a decision that could reshape healthcare for hundreds of millions of people across the continent. They unanimously endorsed the Regional Rehabilitation Strategy 2025–2035 a comprehensive ten-year framework that, for the first time, sets concrete targets for making rehabilitation an essential health service across all 47 African Union member states in the WHO African Region.
The stakes could not be higher. More than 210 million Africans require rehabilitation and approximately two out of three of them currently cannot access it.
What Is Rehabilitation and Why Does It Matter?
Rehabilitation is often misunderstood as something that happens only after accidents. In reality, it is a set of interventions that help people with health conditions including developmental disorders, road traffic injuries, mental health conditions, stroke, cancer, and infectious diseases to function optimally in daily life. It encompasses preventing loss of function, slowing its rate of decline, restoring function where possible, compensating for permanent loss, and maintaining existing function.
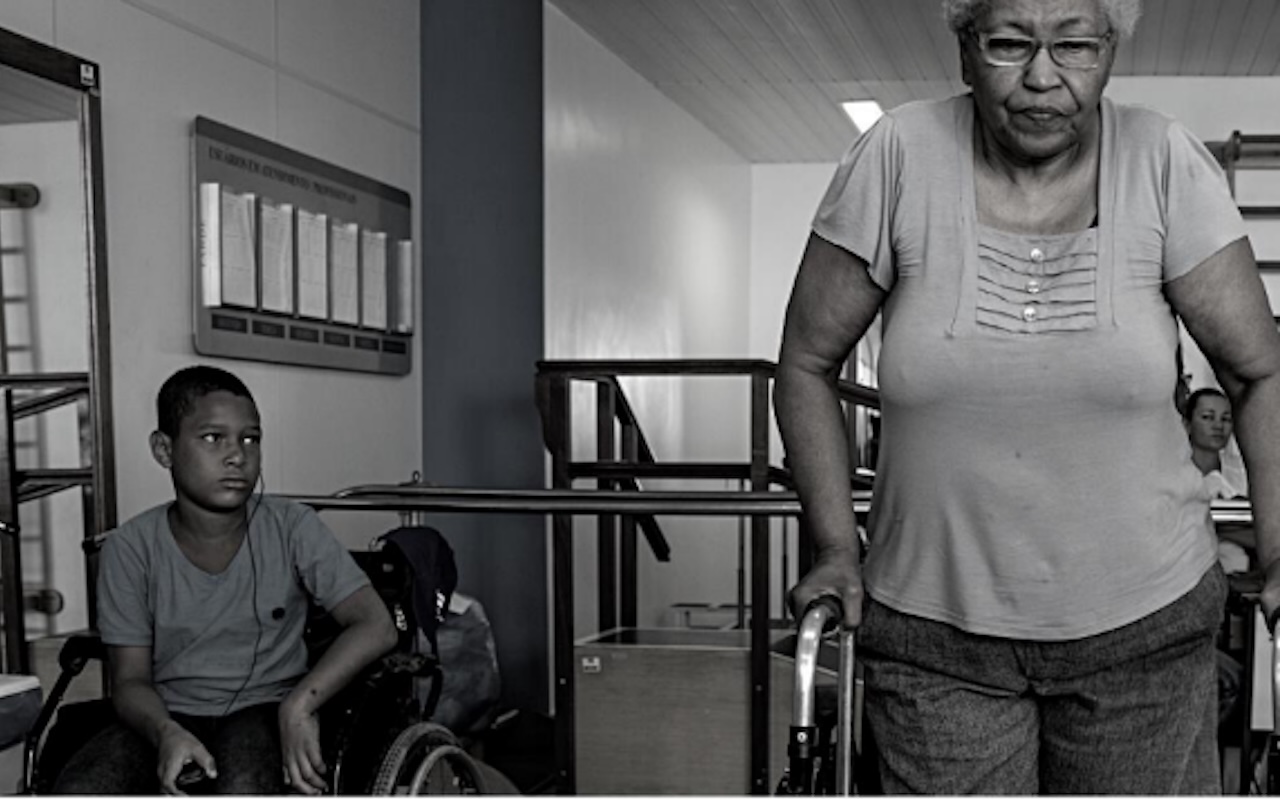
For persons with disabilities, rehabilitation is often the bridge between a diagnosis and a life. A child with cerebral palsy who receives physiotherapy can develop motor skills they would otherwise not achieve. A stroke survivor who accesses occupational therapy can regain the ability to perform daily tasks independently. A person with psychosocial disability who receives community-based mental health support can remain part of their community rather than being institutionalised.
The WHO Africa Region has recorded a 67 percent surge in disability-adjusted life years (DALYs) due to non-communicable diseases, and the lingering effects of conflicts, Ebola, and COVID-19 continue to drive demand for rehabilitation services. Yet health sector expenditure for rehabilitation across most African countries remains very low, fragmented, and heavily dependent on out-of-pocket payments.
The Critical Access Gap
The numbers paint a sobering picture. Sub-Saharan Africa has approximately 0.04 physiotherapists per 10,000 people compared to a global average of 0.7 per 10,000. That means Africa has roughly one-eighteenth of the rehabilitation workforce it needs by global standards.
There are patients in Central Africa who travel more than 1,000 kilometres to access rehabilitation expertise that simply does not exist in their region. Affordability of services and transportation are the two primary barriers that prevent people with disabilities from receiving needed rehabilitation, according to WHO Africa’s own assessments.
The Five Pillars of the 2025–2035 Strategy
The WHO Africa Regional Rehabilitation Strategy 2025–2035 is built around five strategic pillars designed to systematically address these gaps. The strategy targets 60 percent of African countries having national rehabilitation plans with dedicated budgets, and 60 percent of primary health facilities integrating rehabilitation as part of essential health services, by 2035.
- Pillar 1: Leadership and governance embedding rehabilitation in national health policies and budgets
- Pillar 2: Service delivery expanding rehabilitation services from tertiary hospitals to primary health care and community levels
- Pillar 3: Workforce development training more rehabilitation professionals and integrating rehabilitation into medical and nursing curricula
- Pillar 4: Assistive products and technology ensuring availability of wheelchairs, hearing aids, prosthetics, and other essential assistive products
- Pillar 5: Financing developing sustainable funding models including health insurance integration
The strategy also calls for integrating rehabilitation and assistive products into emergency preparedness and response, and for standardised data collection systems so that governments can make evidence-based decisions about rehabilitation investment.
The Education Gap That Threatens the Whole Strategy
Researchers at the University of Dschang in Cameroon and colleagues from Benin and France published a sharp analysis in late 2025 warning that the WHO strategy risks failure without educational reform. Their analysis, published in Frontiers in Medicine, argues that medical schools across Central Africa systematically exclude rehabilitation from undergraduate curricula meaning that doctors, nurses, and other health professionals enter the workforce without any practical knowledge of rehabilitation as a health service.
The consequence is circular: physicians trained without rehabilitation exposure cannot prioritise it in policy, training pipelines remain empty, and community-level rehabilitation services stagnate. The researchers argue that medical curriculum integration is the most cost-effective, scalable intervention available one that would amplify the impact of all five strategy pillars simultaneously.
Currently, only 15 of 47 WHO African Region countries have enacted national rehabilitation governing mechanisms. The strategy’s target of reaching 35 countries by 2035 is ambitious and will require political commitment at the highest levels of health ministries.
WHO’s Disability Inclusion Guide for Action
Alongside the rehabilitation strategy, WHO Africa hosted a multilingual webinar in September 2025 to share lessons learned from implementation of its Disability Inclusion Guide for Action across African countries. The event offered live translations in English, French, and Portuguese recognising the continent’s linguistic diversity and focused on fostering cross-sectoral dialogue on health equity for persons with disabilities. The Guide is designed to help governments make their health systems genuinely accessible, not just nominally so.
📌 Community-based rehabilitation (CBR) programmes remain one of the most effective approaches for reaching persons with disabilities at the local level. The CBR Africa Network (afri-can.org) provides a directory of programmes and resources across the continent.
What This Means for Advocates and OPDs
For disability organisations across Africa, the WHO rehabilitation strategy provides a powerful policy hook for advocacy. When engaging with health ministries, OPDs can now reference a legally endorsed continental framework that commits governments to specific targets. They can demand that national rehabilitation plans be developed with meaningful consultation of persons with disabilities. They can advocate for rehabilitation line items in national health budgets, and they can hold governments accountable through the monitoring mechanisms built into the strategy.
Rehabilitation is not a luxury. It is an essential health service and for 210 million Africans, it is long overdue.




